What is UPNEEQ® (oxymetazoline hydrochloride ophthalmic solution) 0.1%?
- UPNEEQ is the first and only, FDA-approved topical treatment option for low-lying eyelids (acquired ptosis) in adults
- Patients administer UPNEEQ as a once daily drop to each ptotic eye
- It is non-preserved and available in a single-use container that can be stored at room temperature
- Patients should discard the single-use container immediately after dosing
- Contact lenses should be removed prior to instillation of UPNEEQ and may be reinserted 15 minutes after its administration
- If more than one topical ophthalmic drug is being used, the drugs should be administered at least 15 minutes apart
- UPNEEQ is formulated with hypromellose that coats and protects the ocular surface
How does UPNEEQ® work?
- The active ingredient of UPNEEQ is oxymetazoline
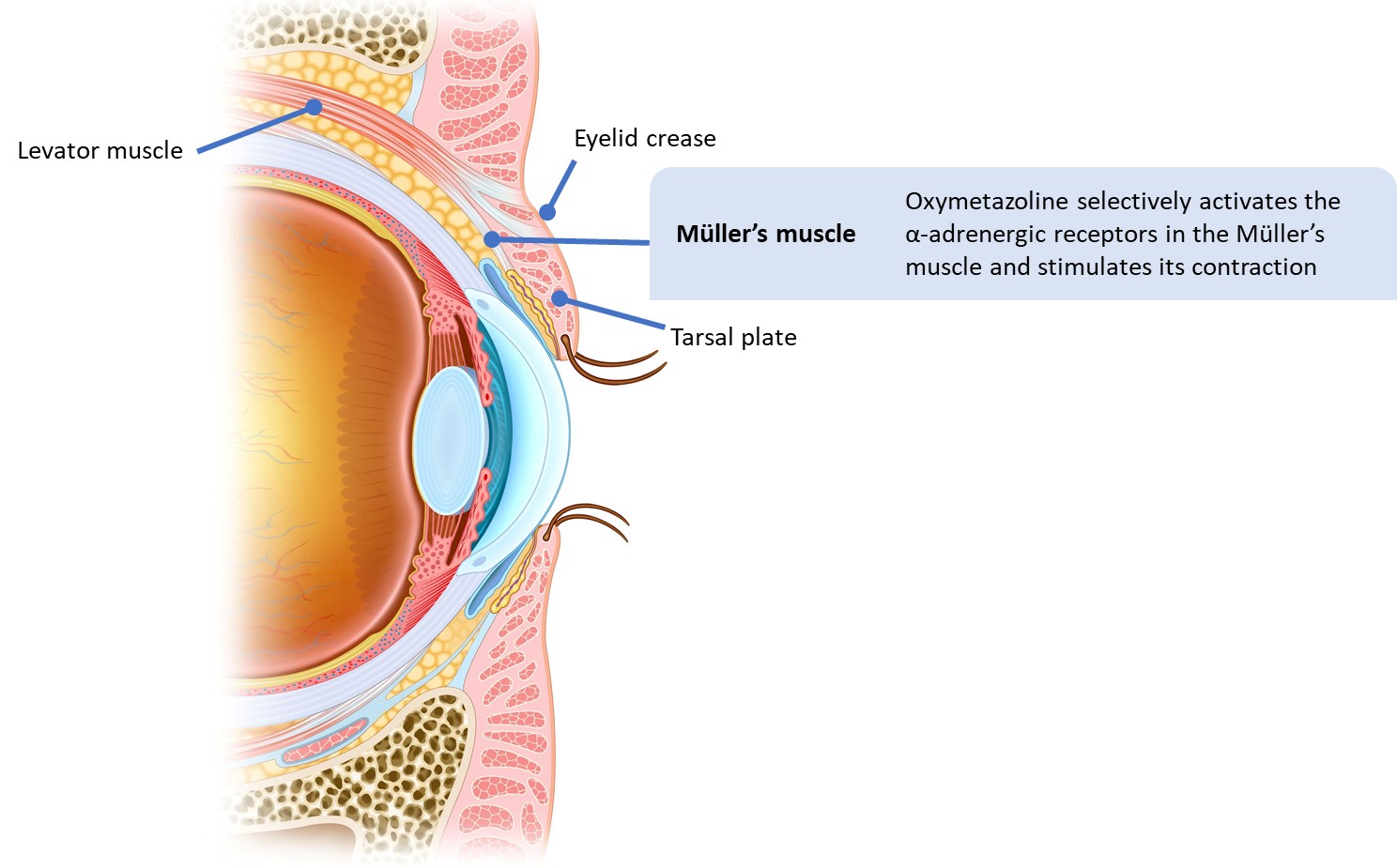
- Oxymetazoline is an α-adrenergic receptor agonist that selectively activates the α-adrenergic receptors in the Müller’s muscle and stimulates its contraction. This elevates the upper eyelid, which decreases lid platform show, reduces the obstruction of the iris, and opens the eye up
Who should be prescribed UPNEEQ?
- UPNEEQ is indicated for the treatment of acquired low-lying eyelids in adults, regardless of the severity of their ptosis
- Low-lying eyelids can be a sign of a more serious underlying condition such as stroke and/or cerebral aneurysm, myasthenia gravis, chronic progressive external ophthalmoplegia (CPEO), Horner’s syndrome, cranial nerve III palsy, orbital infection, and orbital masses. Patients should be appropriately screened by an ophthalmic specialist if a serious underlying condition is suspected
How effective is UPNEEQ®?
- Two randomized, multicenter, double-masked, vehicle-controlled, Phase 3 studies compared once-daily UPNEEQ to vehicle in 304 patients with low-lying eyelids
- The clinical trials showed that the average upper eyelid lift was approximately 1 mm after UPNEEQ instillation
- Upper eyelid lift [as measured by Marginal Reflex Distance (MRD-1)] was significantly improved in the UPNEEQ group as compared to vehicle on Day 1 at 6 hours post-dose and on Day 14 at 2 hours post-dose
- UPNEEQ has been shown to have an observed effect for up to 8 hours after instillation
- Elevation of the eye lid can occur in as little as 5 minutes after instillation
- The clinical trials also showed that UPNEEQ improved superior visual field in patients
- There was a statistically significant visual field improvement from baseline (as measured by the Leicester Peripheral Field Test) in the UPNEEQ group as compared to the vehicle group at 2 hours post-dose on day 14 and maintained at 6 hours post-dose on day 1
- Patients in the clinical trials used UPNEEQ once a day in both eyes for 6 weeks

How safe is UPNEEQ®?
- In the clinical trials, the side effect profile of UPNEEQ was similar to vehicle with no individual adverse reaction occurring in more than 3.5% of patients
- Most adverse reactions were mild and non-treatment-related
- Adverse effects included: punctate keratitis, conjunctival hyperemia, dry eye, blurred vision, instillation site pain, eye irritation and headache
- Warnings and Precautions
- Potential Impacts on Cardiovascular Disease: Alpha-adrenergic agonists may impact blood pressure. UPNEEQ should be used with caution in patients with severe or unstable cardiovascular disease, orthostatic hypotension, and uncontrolled hypertension or hypotension. Advise patients with cardiovascular disease, orthostatic hypotension, and/or uncontrolled hypertension/hypotension to seek immediate medical care if their condition worsens
- Potentiation of Vascular Insufficiency: UPNEEQ should be used with caution in patients with cerebral or coronary insufficiency, or Sjogren’s syndrome. Advise patients to seek immediate medical care if signs and symptoms of potentiation of vascular insufficiency develop
- Risk of Angle Closure Glaucoma: UPNEEQ may increase the risk of angle closure glaucoma in patients with untreated narrow-angle glaucoma. Advise patients to seek immediate medical care if signs and symptoms of acute angle closure glaucoma develop
- Risk of Contamination: Patients should not touch the tip of the single patient-use container to their eye or to any surface, in order to avoid eye injury or contamination of the solution
- Contraindications
- None
References:
- Upneeq® (oxymetazoline hydrochloride ophthalmic solution), 0.1%. [Prescribing Information]. RVL Pharmaceuticals, Inc. 2021.
- Larson T. Artificial tears: a primer. Available at: http://webeye.ophth.uiowa.edu/eyeforum/tutorials/artificial-tears.htm. Accessed October 22, 2020. November 23, 2016.
- Haenisch B, Walstab J, Herberhold S, et al. Alpha-adrenoceptor agonistic activity of oxymetazoline and xylometazoline. Fundam Clin Pharmacol. 2010;24:729-739.
- Sugden D, Anwar N, Klein D. Rat pineal α1-adrenoceptor subtypes: studies using radioligand binding and reverse transcription-polymerase chain reaction analysis. Br J Pharmacol. 1996;118:1246-1252.
- Hosten LO, Snyder C. Over-the-counter ocular decongestants in the United States - mechanisms of action and clinical utility for management of ocular redness. Clin Optom. 2020;12:95-105.
- Slonim CB, Foster S, Jaros M, et al. Association of oxymetazoline hydrochloride, 0.1%, solution administration with visual field in acquired ptosis: a pooled analysis of 2 randomized clinical trials. JAMA Ophthalmol. 2020;138:1168-1175.
- Wirta DL, Korenfeld MS, Foster S, et al. Safety of once-daily oxymetazoline HCl ophthalmic solution, 0.1% in patients with acquired blepharoptosis: results from four randomized, double-masked clinical trials. Clin Ophthalmol. 2021;15:4035-4048.


